Trends
COVID-19 shown to trigger inflammation in the brain: ‘A silent killer
COVID-19 activates the same inflammatory response in the brain as Parkinson’s disease, according to research led by The University of Queensland.
The discovery identified a potential future risk for neurodegenerative conditions in COVID-19 recipients, as well as a potential treatment.
Professor Trent Woodruff and Dr. Eduardo Albornoz Balmaceda from UQ’s School of Biomedical Sciences led the UQ team, which included virologists from the School of Chemistry and Molecular Biosciences.
“We studied the effect of the virus on the brain’s immune cells, ‘microglia’ which are the key cells involved in the progression of brain diseases like Parkinson’s and Alzheimer’s,” Professor Woodruff said.
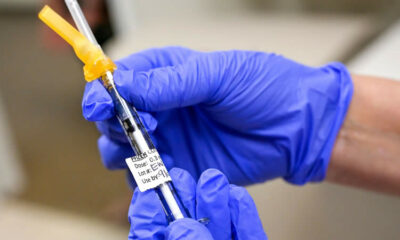
“Our team grew human microglia in the laboratory and infected the cells with SARS-CoV-2, the virus that causes COVID-19.
“We found the cells effectively became ‘angry’, activating the same pathway that Parkinson’s and Alzheimer’s proteins can activate in disease, the inflammasomes.”
According to Dr. Albornoz Balmaceda, activating the inflammasome pathway starts a “fire” in the brain, which starts a chronic and sustained process of killing off neurons.
“It’s kind of a silent killer because you don’t see any outward symptoms for many years,” Dr. Albornoz Balmaceda said.
“It may explain why some people who’ve had COVID-19 are more vulnerable to developing neurological symptoms similar to Parkinson’s disease.”
The researchers discovered that the virus’s spike protein was sufficient to initiate the process, which was exacerbated when there were already proteins in the brain linked to Parkinson’s.
“So if someone is already pre-disposed to Parkinson’s, having COVID-19 could be like pouring more fuel on that ‘fire’ in the brain,” Professor Woodruff said.
“The same would apply for a predisposition for Alzheimer’s and other dementias that have been linked to inflammasomes.”
However, the study discovered a potential treatment.
The researchers used a class of inhibitory drugs developed by UQ that are currently being tested on Parkinson’s patients in clinical trials.
“We found it successfully blocked the inflammatory pathway activated by COVID-19, essentially putting out the fire,” Dr. Albornoz Balmaceda said.
“The drug reduced inflammation in both COVID-19-infected mice and the microglia cells from humans, suggesting a possible treatment approach to prevent neurodegeneration in the future.”
The study is published in Nature’s Molecular Psychiatry.