Trends
Cancer vaccinations already exist, but your doctor may not tell you about them until you ask
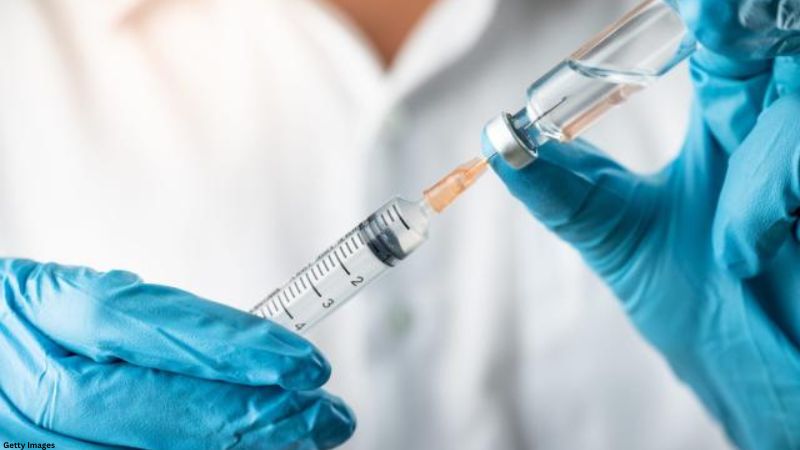
Cancer vaccines are a concept that appears to have been torn from the plot of a futuristic sci-fi movie or the pages of a decades-old utopian novel far ahead of its time. But such scientific wonders do exist now. While there is still more work to be done, they have been preventing cancer and saving lives for more than four decades.
“If you took a poll and asked people, ‘Do we have a vaccine against cancer?’ people would say no,” Karen Knudsen, CEO of the American Cancer Society, tells yahoo. “They really don’t know that we do.”
BioNTech and Moderna made news lately for looking into the possibility of mRNA vaccines, first used with COVID, to treat cancer. Such vaccines use lab-created messengers that teach the body on how to develop an immune response.
However, clinical trials using more standard vaccine technologies have long been underway, and participants are currently getting cancer vaccines, many of which are personalized. The US Food and Drug Administration has previously approved a number of vaccines. Cancer vaccines have been available since the 1980s.
“Patients need to advocate for themselves,” says Dr. Nina Bhardwaj, director of immunotherapy at the Vaccine and Cell Therapy Laboratory and co-director of the Cancer Immunology Program at The Tisch Cancer Institute at the Icahn School of Medicine at Mount Sinai in New York City. We tend to think “the doctor is absolutely right,” she says. “But that’s not always the case, by any means.”
What is a cancer vaccine?
Cancer vaccinations are similar to vaccines for infectious diseases such as the flu, measles, mumps, and COVID, according to Dr. Keith Knutson, a Mayo Clinic immunology professor who studies and develops cancer vaccines. Vaccines stimulate the immune system to fight a specific target, which is generally a virus. The aim in this situation, however, is cancer.
Currently, the majority of cancer vaccines are therapeutic that are used to treat patients who already have advanced disease, frequently in conjunction with additional treatments such as chemotherapy, surgery, or radiation. According to the Cancer Research Institute, two are now authorized by the FDA: one for early-stage bladder cancer and one for prostate cancer.
However, there are vaccinations available for cancer survivors. They’re given to those in remission who are at high risk for recurrence, according to Knutson. He is in charge of a Defense Department-funded project that is testing vaccinations to prevent the return of triple-negative breast cancer.
How do cancer vaccines work?
With a few exceptions, vaccinations for active cancer are now in clinical studies. They are not, however, cures, and acquiring one is far more difficult than visiting a pharmacy and getting a COVID or flu vaccination. Clinical studies for personalized cancer vaccinations are prevalent. However, developing them is a time-consuming process. “Cancer doesn’t wait,” says Dr. Phillip Febbo, chief medical officer of biotechnology company Illumina.
According to Febbo, Illumina is giving genetic sequencing capabilities to Moderna for its melanoma-prevention vaccine, which will be administered to patients who have been diagnosed and had their tumors removed.
Patients who had both their new vaccination and Merck’s Keytruda, a monoclonal antibody medication that helps immune cells attack cancer cells, were 44% less likely to die or have their disease recur, the firms said in December. The medicine is going on to a Phase 3 study, the final step before FDA approval.
“We’re in a new era now, having just seen mRNA vaccines,” Knudsen says. “Is mRNA vaccine technology a new frontier for us? It’s still an open question.”
How to get a cancer vaccine?
Cancer vaccinations have a promising future, according to experts, but not for everyone. All of the experts Fortune spoke with were worried that new medical technologies, such as cancer vaccinations, would disproportionately benefit the wealthy while remaining out of reach for many members of marginalized communities.
It’s a common occurrence in clinical studies in general, and it’s not new in health care, according to Bhardwaj. “The poor or underserved populations are less likely to be included,” she says. Unconscious and intentional biases occur, frequently against non-white patients, women, and the elderly. As a result, doctors may refuse to recommend clinical trials or certain treatments, and “patients need to advocate for themselves,” she says.
Case in point: Black men are around twice as likely to die of prostate cancer than white men. “Some of that is because we don’t understand enough about the genetics of risk,” she says. “But some of it is lack of access to care and clinical trials,” which offer “the most advanced form of care.”
If patients are interested in vaccinations for their cancer, whether approved or in clinical trials, they should not wait for their oncologist to bring it up, according to experts. “Ask, ‘Am I eligible? What would the benefits and concerns be? What are my treatment options?’” Knudsen advises. “Get a second opinion when you can.”
How close are we to the widespread availability of cancer vaccines?
The majority of current cancer vaccinations are for people who have an advanced illness. According to Febbo, it is the “natural progression of medicine” to start with those in the most need. “We make progress, and then we take that progress and march up earlier and earlier in disease stage,” says one researcher.
Knutson predicts that during the next decade, a rising number of therapeutic cancer vaccines will be created. There are numerous active Phase 2 and possibly Phase 3 clinical trials for such things, he notes, so more aid should be on the way relatively soon. Sometimes the problem isn’t a lack of new successful treatments, but rather a lack of funding to see them through to conclusion.
“Part of the problem is and continues to be—in all realms, whether cancer vaccine or some other kind of treatment—that somebody needs to pick up the (cost of the) higher level clinical studies,” like Phase 3 trials, he says.
According to Knutson, “there’s no question a lot of opportunities have been missed” throughout the years. In the worst-case scenario, his team creates a successful cancer vaccine but is unable to fund a Phase 3 study, which is required for FDA approval.